You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Proactive intervention in restorative dentistry is essential in order for the clinician to preemptively deal with hard-tissue breakdown before it requires more painful and complicated procedures. Proactive intervention will benefit the dentist and the patient throughout the various phases of treatment of the patient's lifetime. It will make oral care simpler. Minimally invasive techniques at the onset of tooth structure weakness will mitigate the need for more invasive procedures, such as root canal, later in life.1
The introduction of restorative bioactive materials now makes it easier to control demineralization and potential caries progression, rein in potential damage, and provide a more proactive treatment approach.
Bioactivity
Although bioactivity is a concept that has increased in popularity over the last 5 to 10 years, the term bioactive material was originally introduced in 1969 by Larry Hench, PhD. A bone-grafting material with better bonding capability was needed to treat returning Vietnam veterans who had sustained bone damage. He needed to develop a graft material for bone reconstruction that formed living bonds with the patient's bone. Most materials at the time were rejected by the body and did not bond with the patient's existing bone.2
Hench developed bioglass, a synthetic material that chemically bonded to the bone. At the same time, similar materials for enamel and dentin were developed. Although the definition of bioactivity can change based on the context in which it is used, for the purpose of this article, it is generally defined as something that has an effect on, interaction with, or response from living tissue. Therefore, any time a restorative material interacts with living tissue, it is considered to be bioactive. Before the introduction of bioactive materials, restorative materials such as amalgam and composite resin were used as bandages or placeholders, without controlling the source of the problem.
Caries Management
The goal is to move caries management from a surgical model, which only solves the issue when an invasive procedure is needed, to a medical model, which works to preemptively stop the process of caries before it becomes a more serious condition.
Dental caries is a transmissible bacterial infection, generally caused by Streptococcus mutans or lactobacilli. The infection usually occurs when a child is about 2 or 3 years old and is often transmitted by a parent or caregiver. If transmission occurs, the individual will carry the bacteria in the body throughout life. Diet can also affect caries, particularly a high-sugar diet, which bacteria can "chew" on, potentially inducing an acid attack. Additionally, people with salivary dysfunction may be more caries-prone.3
Strategies to help combat caries include the use of antimicrobials such as fluoride, a healthy diet, good saliva flow, good components within saliva, good oral hygiene such as tongue cleaning, and remineralization from bioactive materials.4
Demineralization and Fluoride
The process of bacteria digesting sugars or carbohydrates is known as the cariogenic challenge. As this process occurs, the resting salivary pH, which starts around 7, begins to decrease. When it reaches the critical level, which is generally around 5.5, the equilibrium is disturbed and demineralization begins to occur. When demineralization occurs, the tooth softens and minerals slowly leach out of the tooth.5 If demineralization continues without intervention, eventually a cavity will form. At this point, a material is needed to restore the tooth to its original form. The goal of bioactive restorative materials is to control the demineralization process and to stop further cavitation in the restored tooth.
When fluoride is applied, fluoridated hydroxyapatite is created and the critical pH drops. As a result, demineralization will only occur when the pH level falls below 4.5, not 5.5.
Saliva in the mouth acts like a bloodstream. Saliva can help build and maintain the health of soft and hard tissues it comes in contact with and will remove waste. It also contains proteins that fight disease and offers first-line protection when fighting microbial invasions. However, a patient suffering from salivary deficiency will have a higher risk for caries, and therefore the practitioner must be proactive in dealing with this condition for the patient.
Building a fluoride reservoir is important in the process of remineralization. A fluoride reservoir is an area where micro-quantities of fluoride can be stored to remineralize the tooth where it is necessary. When fluoride is applied to the teeth, whether through a topical fluoride application or when using a toothpaste containing fluoride, calcium fluoride will precipitate through the mouth. This precipitate is generally stored in plaque and on enamel surfaces. This is called the fluoride reservoir. Consequently, when there is a bacterial challenge or the pH level drops, the fluoride stored will activate and help create fluorapatite to remineralize the teeth.6 When plaque acid occurs, the calcium fluoride-like material in the reservoir dissolves before the enamel, releasing fluoride exactly when and where it is needed. Fluoride works to prevent caries by boosting the ability of the saliva to return lost minerals to the tooth enamel before cavitation can occur.
Bioactive Dental Materials
With the introduction of a variety of bioactive materials, dealing with caries has switched from being a reactive treatment to a preventive treatment. Bioactive materials remineralize actual tooth structure, allowing for prolonged protection from caries and prevention of cavitation.7 Several materials promote remineralization and prevent demineralization, including fluoride, glass ionomers, giomers, and tricalcium-silicate cements.8
Glass-ionomers are beneficial in treating and preventing demineralization in a number of ways: There is no risk of polymerization shrinkage stress as with composite resins. Also, glass-ionomers will attach to affected dentin. This minimizes the amount of tooth that is necessary to remove for restoration. It also protects the margin of a restoration from recurrent caries. The fluoride release will harden carious dentin and encourage formation of caries-resistant dentin, creating a decay-resistant base beneath the restoration.9
However, there are disadvantages to consider before using glass-ionomer cements, including lack of toughness, early water sensitivity, low-abrasion sensitivity, and porosity, ultimately leading to poor surface polish. Because strength of cement is directly related to its water content, early protection of cement from hydration or dehydration is necessary. Light-cured coating materials have largely solved this problem.10 Because of their healing properties, glass-ionomer cements can be used in Class I, II, and V posterior restorations in high caries-risk patients, pediatric patients, geriatric patients, special-needs patients, or patients for whom the lesion location does not allow for a light-cured option.11,12
Another bioactive restorative material shown to be effective for preventing demineralization is the giomer. Giomers combine the benefits of glass-ionomers, particularly fluoride release, with the benefits of composite resins, such as ease of use, strength, and esthetics. Although there are similarities to traditional glass-ionomers, giomers also have advanced esthetic and durability benefits.13 Giomers have the ability to release and recharge fluoride, allowing for continual protection of the tooth. They decrease acid production of cariogenic bacteria, create an acid-resistant layer, and reduce mineral solubility in teeth.14 Additionally, the presence of specific ions in the giomer creates an antiplaque effect by making it more difficult for the plaque to settle on the surface.15
More recently, flowable giomers have been introduced with physical properties that rival traditional hybrid giomers. They come in two viscosities (low flow and no flow)16 and have easier handling, while retaining the benefits of hybrid giomers. Often a disadvantage of flowables is the lack of radiopacity. However, flowable giomers are radiopaque and therefore face no problems in x-ray detection. They are also non-slumping and self-leveling. They hold shape with or without a matrix band. Their viscosity also allows injection of material for easy buildup. Giomers, both hybrid and flowable, can be used for Class I to V restorations.
Another bioactive material is tricalcium-silicate cement, a complete dentin replacement material that can be used to save teeth and potentially avoid endodontic treatment. As with glass-ionomer cements and giomers, this material promotes remineralization. Additionally, it also helps preserve pulp vitality through regeneration of the tooth structure at the root dentin level.17,18 Reactionary dentin bridges are formed in the dentin near the pulp. This promotes pulpal healing in conditions such as pulp exposure, reversible pulpitis, trauma, and many other instances.
Extended-Contact Giomer Varnish
Although fluoride varnishes are helpful, an extended-contact giomer varnish could be considered for patients with sensitivity issues or in high caries-risk areas. Unlike fluoride varnish, which is only in the mouth for a few minutes, leading to efficacy lasting only a few hours, the extended-contact giomer varnish can last 6 months or longer. It is a site-specific, light-cured coating made for both enamel and dentin tooth surfaces.19 It has sustained fluoride, phosphate, and calcium release that is effective over a prolonged period.
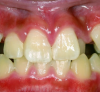
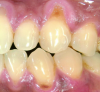
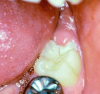
Extended-contact giomer varnish does not require acid etching for uncut enamel. It is a very thin film, so the patient will be less likely to feel it. It can be used for sensitivity or as a proactive intervention on white-spot lesions (Figure 1), exposed root surfaces (Figure 2), and erupting molars (Figure 3). Extended-contact giomer varnish is an ideal solution as a barrier against demineralization and acid erosion, which often occurs in areas that are difficult to clean, like the area around orthodontic brackets.
Case Studies Using Flowable Giomers
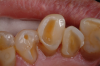
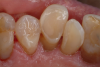
A man in his late 70s presented with worn dentition on his left side (Figure 4). The damage occurred over many years. Treatment options can range from full-mouth rehabilitation to spot-treating areas with a giomer flowable. The decision was made to repair these areas with flowables. Giomer flowables are strong and rival hybrids in their physical properties; therefore, they are effective, esthetically pleasing, and easier to use. The direct restorative approach is also a very cost-effective option.
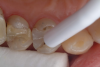
First, the affected areas were lightly roughened with a bur and bonded with a bonding agent. Then anatomy was created by flowing the materials into the affected areas, followed by polishing (Figure 5). Now, a few years later, the patient's teeth are beginning to show a bit of wear, but the treatment worked very well, and he may not need another procedure like this for several years, if ever. If he needs another procedure, it will only take a few minutes. As wear begins, it will be treated proactively and be easily maintained for the rest of his life.
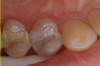
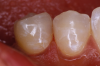
Another case involved a breakdown of the margins of a tooth on the upper left side. There was staining and a bit of decay (Figure 6). First, a fissurotomy bur was used to remove the staining and decay and prepare the tooth for a restoration. Next, the tooth was bonded, dried, and cured, and a flowable giomer was placed (Figure 7). The flowable giomer worked to fill in gaps, as well as to help remineralize the tooth. This gave the patient a serviceable restoration without the trauma of complete replacement.
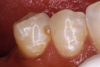
In the next case, the decay was cleaned out from the buccal surface as opposed to the occlusal, eliminating the need to remove the marginal ridge (Figure 8). Then the flowable was applied, with the restoration treated as a Class III (Figure 9). The advantage of not removing the marginal ridge was that it preserved the integrity and longevity of the tooth.
Conclusion
In conclusion, changing from a surgical model to a medical model has changed the way dentists deal with caries. Instead of waiting to treat, dentists can proactively intervene before the demineralization process becomes irreversible. Through the use of remineralization therapies and bioactive materials, dentists may avoid the need for more invasive treatments and help their patients keep their teeth for a lifetime.
About the Author
Fay Goldstep, DDS
Private Practice
Richmond Hill, Ontario, Canada
References
1. Goldstep F. Proactive intervention dentistry: a model for oral care through life. Compend Contin Educ Dent. 2012;33(6):398-402.
2. Jones JR. Review of bioactive glass: from Hench to hybrids. Acta Biomater. 2013;9(1):4457-4486.
3. Maheswari SU, Raja J, Kumar A, Seelan RG. Caries management by risk assessment: a review on current strategies for caries prevention and management. J Pharm Bioallied Sci. 2015;7(suppl 2):S320-S324.
4. Arteaga S. Demineralization and remineralization: the battle to keep teeth strong and healthy. Dentistry IQ. http://www.dentistryiq.com/articles/wdj/print/volume-4/issue-9/focus-on-orthodontics/demineralization-and-remineralization-the-battle-to-keep-teeth-strong-and-healthy.html. Published October 1, 2006. Accessed June 5, 2018.
5. Abou Neel EA, Aljabo A, Strange A, et al. Demineralization-remineralization dynamics in teeth and bone. Int J Nanomedicine. 2016;11:4743-4763.
6.Vogel GL. Oral fluoride reservoirs and the prevention of dental caries. Monogr Oral Sci. 2011;22:146-157.
7. Tooth repair the bioactive way. Shofu. http://www.shofu.com/en/wp-content/uploads/sites/2/2014/05/Inside-Dentistry-Tooth-Repair-the-Bioactive-Way-E-Book.pdf. Inside Dent. Published January 2017. Accessed June 5, 2018.
8. Chen L, Shen H, Suh BI. Bioactive dental restorative materials: a review. Am J Dent. 2013;26(4):219-227.
9. Knight GM. Glass ionomers: why, where and how. Oral Health. https://www.oralhealthgroup.com/features/glass-ionomers-why-where-and-how/. Published January 11, 2018. Accessed June 5, 2018.
10. McLean JW. The clinical use of glass-ionomer cements-future and current developments. Clin Mater. 1991;7(4):283-288.
11. Ward DH. 20 tips for using glass ionomers. J Cosmet Dent. 2011;27(3):1-80. https://www.aacd.com/proxy/files/Students%20and%20Faculty/20%20tips%20Glass%20Ionomers.pdf. Accessed June 5, 2018.
12. Strassler HE. Glass ionomers for direct-placement restorations. Dental Academy of CE. https://www.dentalacademyofce.com/courses/2052/PDF/1104cei_glassionomer_web.pdf. Published February 2011. Accessed June 5, 2018.
13. Margolis FS. Using Giomers in pediatric care. Inside Dent. 2011;7(10):106.
14. Giomer technology. Shofu. http://www.shofu.com/shofu_images/Literature/giomer%20brochure.pdf. Accessed June 5, 2018.
15. Flax H. Bioactive dentistry with Giomers. Oral Health. https://www.oralhealthgroup.com/features/bioactive-dentistry-giomers/. Published January 11, 2018. Accessed June 5, 2018.
16. Giomer concept. Giomer. http://www.giomer.com/professional/?opt1=concept. Accessed June 5, 2018.
17. Villat C, Grosgogeat B, Seux D, Farge P. Conservative approach of a symptomatic carious immature permanent tooth using a tricalcium silicate cement (Biodentine): a case report. Restor Dent Endod. 2013;38(4):258-262.
18. Watson TF, Atmeh AR, Sajini S, et al. Present and future of glass-ionomers and calcium-silicate cements as bioactive materials in dentistry: biophotonics-based interfacial analyses in health and disease. Dent Mater. 2014;30(1):50-61.
19. Halabo S. Giomer varnish for prolonged hypersensitivity relief. Oral Health. https://www.oralhealthgroup.com/features/1003918293/. Published December 7, 2015. Accessed July 23, 2018.